AESTHETIC PLASTIC
RECONSTRUCTIVE
SURGERY
SEBASTIEN GARSON M.D
LIPOSTRUCTURE
This fact sheet was developed under the aegis of the French Society of Plastic Reconstructive and Aesthetic Surgery (SOF.CPRE) as an addition to your initial consultation, to try to answer all the questions you can ask yourself if you plan to use surgery baldness. The purpose of this document is to provide you with all the necessary and essential elements of information to help you make your decision with full knowledge of the facts. Also you is it advisable to read with the greatest attention.
• DEFINITION OBJECTIVES AND PRINCIPLES
Breast hypoplasia is defined as a volume of breasts that are insufficiently developed in relation to the patient's morphology. It can be the consequence of an insufficient development of the gland at puberty, or appear secondarily by loss of glandular volume (pregnancy, weight loss, hormonal disturbances ... ).
Lack of volume can also be associated with ptosis (drooping breasts with sagging of the gland, distension of the skin and too low areolas).
The operation can be performed at any age from 18 years old.
This hypotrophy is often poorly accepted physically and psychologically by the patient, who experiences it as an attack on her femininity, with the corollary of an alteration in self-confidence and a feeling of unease, sometimes profound, which can go as far as a real complex. This is why the operation aims to increase the volume of breasts considered too small by implanting prostheses.
These sometimes major physical alterations, as well as the psychic suffering induced, give a therapeutic purpose to this restorative surgical act.
A minor patient is usually not considered suitable for an aesthetic breast augmentation. It is however possible in cases of severe hypoplasia or in the context of malformative abnormalities such as breasts.
"tuberous" or "mammary agenesis".
This purely aesthetic surgery cannot be covered by health insurance. Only a few rare cases of true breast agenesis (radical absence of any breast development) can sometimes hope for social security participation after prior agreement.
Breast implants currently in use are composed of an envelope and a filling product.
The shell is in all cases made of a silicone elastomer. This membrane can be smooth or textured (rough). Some contain polyurethane.
The content is the filler in the envelope.
Physiological liquid prostheses, the only ones authorised in France from 1995 to 2001, contain physiological serum (salt water) which is completely harmless. They are either pre-filled in the factory or inflated by the surgeon during the operation, allowing a certain intraoperative volume adaptation.
Prostheses pre-filled with silicone gel are increasingly used. They provide a flexible feel to the breast that is close to a natural consistency. The gels are more or less cohesive. Cohesiveness limits perspiration, i.e. the "sweating" of the gel through the wall, a possible source of the shell. It prevents, in case of rupture, the diffusion of silicone.
The shape Alongside the classic round prostheses ensuring a beautiful cleavage, there are profiled "drop-shaped" prostheses called anatomical for a more natural look of the breast.
This great variety of shape and volume allows the choice of prostheses to be optimised and adapted, almost "made to measure", according to the patient's morphology and personal expectations.
Constant evolution is aimed at improving the watertightness and solidity of the walls, the palpatory and visual naturalness of the rendering, the durability and tolerance of the materials.
In any case, to this day, all implants available in France are subject to precise and rigorous standards: CE marking (European Community) and authorization by the ANSM (National Agency for the Safety of Medicines and Health Products).
In addition, the French administrative authorities and the Ministry of Health have imposed, since November 2016, the establishment of a national register of breast prostheses.
This register will remain completely anonymous. Its objective is to list all the implants implanted on French territory and to ensure the monitoring of all implants, which will lead to greater safety for patients.
Other Implants:
Hydrogel-filled prostheses: This is an aqueous gel, registered since 2005, composed largely of water gelled by a cellulose derivative. This gel, of a more natural consistency than physiological serum, is also resorbable by the body in case of rupture of the envelope.
Finally, there are prostheses whose silicone envelope is covered with a polyurethane foam that will be
"embedded" in the surrounding tissue. They therefore provide a form of tissue "grip" that can be interesting in certain difficult cases. The harmlessness of polyurethane is now clearly accepted, and these implants have experienced a certain boom in recent years because they make it possible to better maintain their positioning, reduce the excess weight induced on the lower pole of the breast and prevent the rotation of the anatomical implants. The risk of inducing a shell phenomenon is finally considered to be lower. However, they present a certain number of disadvantages and difficulties of use that will have to be weighed up.
In all cases the choice of the type of prosthesis will be the result of a discussion with the Surgeon who will advise you on the most judicious choice in your particular case.
Since April 4, 2019, the ANSM has withdrawn from the French market the implants whose envelope is called Biocell®, macrotexture or polyurethane.
• BEFORE THE OPERATION
An interrogation followed by a careful examination will have been carried out by the surgeon who will take into account all the parameters that make each patient a particular case (height, weight, pregnancy, breastfeeding, thoracic and mammary morphology, skin quality, importance of the fat and the gland present, musculature ...
Depending on this anatomical context, the surgeon's preferences and habits, and the wishes expressed by the patient, an operating strategy will have been agreed upon. The location of the scars, the type and size of the implants as well as their positioning in relation to the muscle will be predetermined (see below).
A preoperative blood test will be carried out as prescribed. The anaesthetist will be seen in consultation, at the latest 48 hours before the operation. A radiological check-up of the breast is prescribed (mammography, ultrasound).
THE TOBACCO ISSUE
The scientific evidence is currently unanimous about the harmful effects of smoking in the weeks surrounding surgery. These effects are multiple and can lead to major scarring complications, surgical failures and infection of implantable devices (e.g. breast implants).
For procedures involving skin detachment such as abdominoplasty, breast surgery or cervicofacial lifting, smoking can also cause serious skin complications. In addition to the risks directly related to the surgical procedure, smoking can be responsible for respiratory or cardiac complications during anesthesia.
With this in mind, the community of plastic surgeons agrees on a request for complete cessation of smoking at least one month before surgery and then until healing (usually 15 days after surgery). The electronic cigarette should be considered in the same way.
If you smoke, talk to your surgeon and your anesthesiologist. A prescription for nicotine substitute may be offered. You can also get help from Tabac-lnfo-Service (3989) to refer you to a smoking cessation or to be helped by a tobaccologist.
On the day of the operation, if there is any doubt, you may be asked to take a urine nicotine test and if positive, the operation may be cancelled by the surgeon.
• TYPE OF ANESTHESIA AND CONDITIONS OF INTERVENTION
Type of anaesthesia:
This is usually a classical general anaesthesia, during which you sleep completely. In rare cases, however, a 'vigil' anaesthesia (deep local anaesthesia with intravenously administered tranquillizers) may be used (to be discussed with the surgeon and anaesthetist).
Hospitalization arrangements:
The procedure usually justifies a one-day hospital stay. Admission is then in the morning (or sometimes the day before in the afternoon) and discharge is authorized the next day.
However, in some cases, the operation can be performed on an "outpatient" basis, i.e. with discharge the same day after a few hours of supervision..
• INTERVENTION
Each surgeon adopts a technique that is specific to him and that he adapts to each case to obtain the best results. However, there are some common basic principles:
Skin incisions:
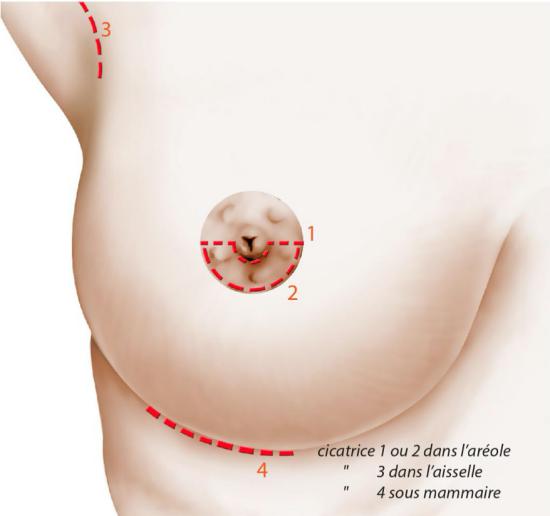
There are several possible "approaches":
areolar routes, with an incision in the lower segment of the circumference of the areola, or a horizontal opening around the nipple from below (1 and 2);
axillary route, with incision under the arm, in the armpit (3);
submammary route, with incision in the groove under the breast (4).
These incisions will of course correspond to the location of the future scars, which will therefore be hidden in areas where they meet or in natural folds.
Fitting of prostheses
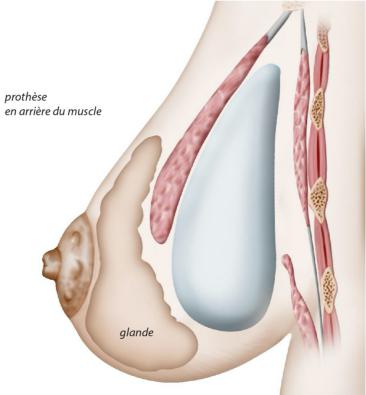
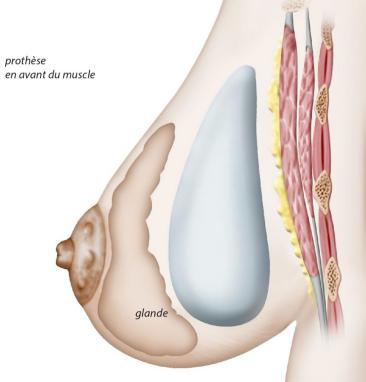
Through the incisions, the implants can then be inserted into the completed boxes. Two positions are possible:
premuscular, where the prostheses are placed directly behind the gland, in front of the pectoral muscles;
Retromuscular, where the prostheses are placed deeper, behind the pectoral muscles. The respective disadvantages will have been discussed with your surgeon.
Complementary gestures
In case of associated breast ptosis (drooping breasts, low areolas), it has been seen that it may be desirable to reduce the skin envelope of the breast in order to make it rise ("mastopexy"). This skin resection will then result in larger scars (around the areola± vertical
± horizontal in the submammary groove)
Drains and dressing
A small drain can be put in place depending on the surgeon's habits and local conditions. It is a device designed to evacuate the blood that could accumulate around the prostheses.
At the end of the operation, a 'shaping' dressing is made with an elastic bandage.
Depending on the surgeon, the approach and the possible need for additional associated procedures, the operation can last from one hour to two and a half hours..
AFTER THE INTERVENTION: THE OPERATING SUITES
The post-operative period can sometimes be painful during the first days, especially when the implants are large and especially if they are placed behind the muscles. An analgesic treatment, adapted to the intensity of the pain, will be prescribed for a few days. In the best case, the patient will feel a strong sensation of tension.
Edema (swelling), bruising and discomfort when raising the arms are common in the early stages.
The first dressing is removed after a few days. It is then replaced by a lighter bandage. A bra may then be recommended night and day for a few weeks.
Most of the time, the stitches are internal and absorbable. Otherwise, they will be removed after a few days.
It is advisable to consider a convalescence with interruption of activity for five to ten days.
It is advisable to wait one to two months before resuming sports activities..
• THE RESULT
A period of two to three months is necessary to assess the final result. This is the time needed for the breasts to regain their full flexibility and for the prostheses to stabilize.
The intervention will have allowed an improvement in the volume and shape of the breasts. The scars are usually very discreet. The gain in breast volume has an impact on the overall silhouette, allowing greater freedom of dress. Beyond these physical improvements, the recovery of full femininity often has a very beneficial effect on a psychological level.
The goal of this surgery is to bring an improvement and not to achieve perfection. If your wishes are realistic, the result obtained should give you great satisfaction.
Stability of the result
Regardless of the life span of the prostheses (see below) and with the exception of the occurrence of a significant weight change, the volume of the breasts will remain stable in the long term.
However, as regards the shape and "fit" of the breasts, like natural breasts, the "augmented" breasts will suffer the effects of gravity and ageing, with variable speed depending on the age and support qualities of the skin, but also on the volume of the implants.
• FAULTS OF THE RESULT
Some imperfections may occasionally occur:
a residual volume asymmetry, incompletely corrected despite different sized implants;
a firmness a little too great with flexibility and mobility judged insufficient (especially with large implants);
a somewhat artificial appearance, especially in very thin patients, with too much visibility of the edges of the prosthesis, especially in the upper segment;
Perceptibility to the touch of the implants is always possible, especially when the thickness of the tissue cover (skin + fat + gland) covering the prosthesis is low. This direct palpation of the prosthetic membrane, or even of folds, is more frequent in thin patients, with large volume implants filled with pysiological serum and
in a prepectoral position.
Aggravation of breast ptosis may be observed, especially when large implants are used.
In case of dissatisfaction, some of these imperfections may be corrected surgically after a few months.
MISCELLANEOUS QUESTIONS
Pregnancy/breastfeeding
After the insertion of breast implants, a pregnancy is possible without any danger for the patient or the child, but it is recommended to wait at least six months after the operation. Breastfeeding is not dangerous either and remains possible in most cases.
Autoimmune diseases
The very numerous large-scale international scientific studies carried out on this subject have unanimously demonstrated that there is no greater risk of occurrence of this type of rare disease in patients with implants (especially silicone implants) than in the general female population.
Prostheses and cancer
Until recently, the state of science suggested that the implantation of breast implants, including silicone implants, did not increase the risk of breast cancer. This is indeed still the case for by far the most frequent breast cancers (adeno-carcinomas) whose incidence is not increased by the implantation of a breast prosthesis.
However, in the context of cancer screening after implantation, clinical examination and palpation may be disrupted, especially in the case of a periprosthetic shell or siliconoma. Similarly, the presence of implants can hinder the performance and interpretation of screening mammograms to be done regularly. li must therefore systematically specify that you are a breast implant wearer. Thus, certain specialized radiological techniques (special incidences, digital images, ultrasound, MRI, etc.) may be used depending on the case. In addition, in case of doubt about the diagnosis of breast cancer, it should be noted that the presence of prostheses may require a more invasive exploration to obtain diagnostic certainty.
Large Cell Anaplastic Lymphoma (LAGC) associated with Breast Implants (BIA-ALCL) is a very exceptional clinical entity that has been observed in France since January 2011. This entity mainly concerns implants with a macro-textured surface. It should be sought only in case of proven clinical signs (recurrent peri-prosthetic effusion, breast redness, breast volume increase, perceptible mass). A precise senological assessment must then be carried out in order to specify the nature of the lesion. In nearly 90% of cases, this entity has a very good prognosis and usually heals by an adapted surgical treatment associating the removal of the prosthesis and the peri-prosthetic capsule (total and complete capsulectomy). In about 10% of cases, the pathology is more serious and requires management by chemotherapy and/or radiotherapy within a team specialized in the treatment of lymphomas.
- Intracapsular squamous cell carcinoma is a very exceptional entity (only a few cases published worldwide). In published observations, it occurs in complex cases requiring several interventions and several prosthesis changes.
Lifetime of implants
Even though some patients may keep their implants for decades without major changes, breast implants should not be considered "lifetime" permanent. Thus, an implant-wearing patient can expect to one day have to replace her implants in order to maintain the beneficial effect. The life expectancy of implants, whatever they are, is uncertain and it is impossible to estimate precisely since it depends on wear and tear phenomena of varying speed. The life expectancy of implants can therefore in no way be guaranteed. The average life expectancy is estimated at around 10 years.
It should be noted, however, that the new generation implants have made great progress in terms of resistance and reliability. From the tenth year onwards, the question of changing the prosthesis will have to be asked if there is a change in consistency.
Monitoring
It is essential to undergo the check-ups scheduled by your surgeon in the weeks and months following implantation. Afterwards, the presence of the implants does not remove the need for the usual medical supervision (gynaecological follow-up and breast cancer screening), even if it does not necessitate examinations in addition to those related to this supervision. It is nevertheless essential to specify to the various doctors involved that you are a breast prosthesis wearer.
A monitoring consultation, specific to implants, with your plastic surgeon is recommended every two to three years, but, apart from this monitoring, it is especially fundamental to come and consult as soon as a modification of one or both breasts is detected or after a violent trauma.
Breast ultrasound is a non-irradiating and very efficient examination to judge the integrity of the prosthesis. An ultrasound must be performed at the slightest clinical doubt and for some people systematically once a year.
The prosthetic change is only considered in case of clinical or radiological abnormality or at the request of the patient. It is not always necessary to wait for a certain period of time before changing the prosthesis.
• POSSIBLE COMPLICATIONS
Breast augmentation with prostheses, although carried out for essentially aesthetic reasons, is nonetheless a real surgical procedure, which implies the risks inherent in any medical procedure, however minor it may be.
This procedure is subject to the risks associated with living tissue, whose reactions are never entirely predictable.
A distinction must be made between complications related to anaesthesia and those related to the surgical procedure:
As far as anaesthesia is concerned, during the obligatory preoperative consultation, the anaesthetist will inform the patient himself of the anaesthetic risks. It is important to know that anesthesia, whatever it is, induces in the organism
sometimes unpredictable and more or less easy to react to
control.
However, by using a competent anaesthetist/resuscitator, working in a real surgical context, the risks involved have become statistically very low. Indeed, it must be borne in mind that techniques, anaesthetic products and monitoring methods have made huge progress over the last thirty years, offering optimal safety, especially when the operation is carried out outside the emergency room and in a healthy person;
as far as the surgical procedure is concerned, by choosing a qualified and competent plastic surgeon, trained for this type of intervention, you limit these risks as much as possible, without however completely eliminating them.
In practice, the vast majority of breast augmentation operations carried out correctly are carried out without any problems, the after-effects are simple and patients are fully satisfied with their results. However, sometimes complications may arise during the operation, some inherent to the breast surgery procedure and others specifically related to the implants:
Complications inherent to breast surgery.
Spills, infection
haematoma: accumulation of blood around the prosthesis is an early complication that can occur in the first few hours. If it is significant, a repeat operation in the operating room is then preferable in order to evacuate the blood and stop the bleeding at its origin;
Serous effusion: an accumulation of lym phatic liquid around the prosthesis is a frequent phenomenon in the immediate post-operative period. It is often associated with edema. It results in a transient increase in breast volume. It disappears spontaneously and gradually;
At a distance from the surgery, a seroma must imperatively lead you to consult your surgeon.
infection: rare after this type of surgery. It may not be resolved by antibiotic treatment alone and then requires a surgical resumption for drainage and removal of the implant for a few months (time needed before a new prosthesis can be put back in place without risk).
There are also three other particular forms of infection:
Late "low noise" infection: this is an infection with few symptoms and without obvious translation on examination, which can sometimes occur several years after implantation;
microabcesses: more common, they develop on a stitch and resolve quickly after removal of the suture and local care;
staphylococcal toxic shock: extremely rare cases of this brutal generalized infectious syndrome have been reported.
Skin necrosis
It is the result of a lack of tissue oxygenation due to localized insufficient blood supply, which may be promoted by excessive tension, haematoma, infection or heavy smoking in the patient. li
a very rare but feared complication because, in the extreme, it can locally expose the prosthesis, in particular by a disunion of the sutures. Surgical revision is often necessary, sometimes with the need to temporarily remove the implant.
Abnormalities of cicatrization
As the healing process involves fairly random phenomena, it sometimes happens that the scars are not as discreet as expected in the long term, and may then take on very variable aspects: enlarged, retractile, adherent, hyper or hypopigmented, hypertrophic (swollen), or even exceptionally keloid.
Altered sensitivity
They are frequent during the first months but most of the time end up regressing. Rarely, however, some degree of dysesthesia (decreased or exaggerated sensitivity to touch) may persist, particularly in the areola and nipple area.
Galactorrhea/lactal spillage
Very rare cases of unexplained postoperative hormonal stimulation have been reported, resulting in milk secretion ("galactorrhea") with sometimes a collection of fluid around the prosthesis.
Pneumothorax
Rarely will he receive specific treatment.
Risks specifically related to implants
Formation of "folds" or the appearance of "waves".
As implants are flexible, it is possible that their envelope may crease and that these creases are perceptible to the touch, or even visible under the skin in certain positions, giving the appearance of waves.
This phenomenon, which is slightly more common with the physiological saline than with silicone gel, occurs mainly in thin patients. A lipomodelling procedure can sometimes be proposed. It consists of applying a thin layer of fat under the skin of the breast in order to "camouflage" the implant.
"Shells
The normal and constant physiological reaction of the human organism in the presence of a foreign body is to isolate it from the surrounding tissues by forming a hermetic membrane that will surround the implant and is called a "periprosthetic capsule". Normally, this membrane is thin, flexible and imperceptible, but sometimes the reaction folds and the capsule thickens, becomes fibrous and retracts by compressing the implant, taking the name of "periprosthetic capsule".
"hull". Depending on the intensity of the phenomenon, it can result in: a simple firming of the breast, a constriction sometimes embarrassing, or even a visible deformation with globulisation of the prosthesis leading to an extreme hard, painful, more or less off-centre sphere.
This retractile fibrosis is sometimes secondary to a haematoma or an infection, but most of the time its occurrence remains unpredictable, resulting from random organic reactions.
Much progress has been made in recent years in surgical techniques, but above all in the design and construction of implants (cohesive gel, wall texture) leading to a very significant reduction in the rate and intensity of blistering. If necessary, a reoperation can correct such a contracture by section of the capsule ("capsulotomy"). Polyurethane-coated prostheses can be a solution in case of recurrent shells.
Rupture
We have seen that implants cannot be considered definitive with an average life span of around 10 years. A loss of tightness of the envelope may therefore occur in the long term. This may be simple porosity, punctiform openings, micro-cracks, or even real breaches. Very rarely, it can be the consequence of a violent trauma or an accidental puncture, and much more often it can be the result of progressive wear of the wall due to age.
In any case, this is a possible outcome of the prosthesis filler, with different consequences depending on the nature of the contents:
with saline or absorbable hydrogel, there is partial or total deflation, fast or slow;
with the silicone gel (non resorbable), it will remain contained within the membrane that insulates the prosthesis.
This can then promote the appearance of a shell, but can also remain inconsequential and go unnoticed.
In some cases, which have become much rarer (in particular because of the better "cohesiveness" of current gels), the gel may however gradually penetrate into the surrounding tissues (siliconome).
Prosthetic rupture requires an intervention aimed at
change the implants.
Malposition, displacement
Incorrect positioning, or secondary displacement of the implants, which then affects the shape of the breast, can sometimes justify surgical correction.
Rotation
Although relatively rare in practice, the pivoting of an 'anatomical' prosthesis remains theoretically possible and can affect the aesthetic result.
Deformation of the chest wall
In rare cases, prostheses with fibrous shells, left in place for a long time, can "imprint" themselves in the tissue, leaving a deformation of the chest wall that is difficult to correct when they are removed.
-Late peri-prosthetic seroma
In very rare cases, fluid build-up may occur late around the prosthesis. Such a late effusion, especially if it is associated with other clinical abnormalities of the breast, requires a senological assessment by a specialized radiologist to perform a puncture under ultrasound for analysis. In case of breast mass or recurrent effusion, a surgical exploration will allow a histological analysis of the peri-prosthetic capsule in order to eliminate an exceptional Large Cell Anaplastic Lymphoma Associated with Breast Implants (LAGC-AIM), or an even more exceptional intracapsular pathology such as intracapsular squamous carninoma.
In total there should not overstate the risks, but just be aware that surgery, even seemingly simple, still a small share of hazards. The use of a qualified Plastic Surgeon ensures that it has the training and knowledge required to avoid these complications, or effectively treat if jurisdiction.
These are the pieces of information that we wanted to bring you in addition to the consultation. We recommend that you keep this document, read it again after the consultation and reflect "a clear head." This reflection may raise new questions for which you wait for additional information. We are available to talk during the next consultation, or by phone, or even on the day of surgery when we meet in any way before anesthesia.
CONTACT
Contact Us
Phone : + 33344282959
Address:
7 impasse de la Passerelle 60300 SENLIS
France
Copyright SELARL Dr Garson Pages d'information- Crédits photos : Dr Garson / Libre de droits - Mentions légales
Ce site utilise des cookies à des fins statistiques - Pour en savoir plus, cliquez ICI.
SITE RÉALISÉ AVEC WEBACAPPELLA RESPONSIVE